Pregnancy SmartSiteTM
Loss of bladder control; Uncontrollable urination; Urination - uncontrollable; Incontinence - urinary; Overactive bladder DefinitionUrinary (or bladder) incontinence occurs when you are not able to keep urine from leaking out of your urethra. The urethra is the tube that carries urine out of your body from your bladder. You may leak urine from time to time. Or, you may not be able to hold any urine. The three main types of urinary incontinence are:
Mixed incontinence occurs when you have more than one type of incontinence, usually both stress and urge urinary incontinence. Bowel incontinence is when you are unable to control the passage of stool. It is not covered in this article. CausesCauses of urinary incontinence include:
Incontinence may be sudden and go away after a short period of time. Or, it may continue long-term. Causes of sudden or temporary incontinence include:
Causes that may be more long-term include:
Home CareIf you have symptoms of incontinence, see your health care provider for evaluation, tests, and a treatment plan. Which treatment you get depends on what caused your incontinence and what type you have. There are several treatment approaches for urinary incontinence: Lifestyle changes. These changes may help improve incontinence. You may need to make these changes along with other treatments.
For urine leaks, wear absorbent pads or undergarments. There are many well-designed products that no one else will notice. Bladder training and pelvic floor exercises. Bladder retraining helps you gain better control over your bladder. Kegel exercises can help strengthen the muscles of your pelvic floor. Your provider can show you how to do them. Many women do not do these exercises correctly, even if they believe they are doing them correctly. Often, people benefit from formal bladder strengthening and retraining with a pelvic floor specialist. Medicines. Depending on the type of incontinence you have, your provider may prescribe one or more medicines. These medicines help prevent bladder muscle spasms, relax the bladder, and improve bladder function. Your provider can help you learn how to take these medicines and manage their side effects. Surgery. If other treatments do not work, or you have severe incontinence, your provider may recommend surgery. The type of surgery you have will depend on:
If you have overflow incontinence or you cannot fully empty your bladder, you may need to use a urinary catheter. You may use a catheter that stays in your bladder long-term, or one that you are taught to put in and take out yourself. Bladder nerve stimulation. Urge incontinence and urinary frequency can sometimes be treated by electrical nerve stimulation. Pulses of electricity are used to reprogram bladder reflexes. In one technique, the provider inserts a stimulator through the skin near a nerve in the leg. This is done weekly in the provider's office. Another method uses battery-operated implanted device similar to a pacemaker that is placed under the skin in the lower back. Botox injections. Urge incontinence can sometimes be treated with an injection of onabotulinum A toxin (also known as Botox). The injection relaxes the bladder muscle and increases the storage capacity of the bladder. The injection is delivered through a thin tube with a camera on the end (cystoscope). In most cases, the procedure can be done in the provider's office. When to Contact a Medical ProfessionalTalk to your provider about incontinence. Some providers who treat incontinence are gynecologists and urologists that specialize in this problem. They can find the cause and recommend treatments. Call your local emergency number (such as 911) or go to an emergency room if you suddenly lose control over urine and you have:
Contact your provider if you have:
ReferencesHeesakkers JPFA, Blok B. Electrical stimulation and neuromodulation in storage and emptying failure. In: Partin AW, Dmochowski RR, Kavoussi LR , Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 122. Lentz GM, Miller JL. Lower urinary tract function and disorders: physiology of micturition, voiding dysfunction, urinary incontinence, urinary tract infections, and painful bladder syndrome. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 21. Newman DK, Burgio KL. Conservative management of urinary incontinence: behavioral and pelvic floor therapy, urethral and pelvic devices. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 121. Resnick NM, DuBeau CE. Urinary incontinence. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 115. Reynolds WS, Dmochowski R, Karram MM, Mahdy A. Surgical management of refractory overactive bladder and detrusor compliance abnormalities. In: Baggish MS, Karram MM, eds. Atlas of Pelvic Anatomy and Gynecologic Surgery. 5th ed. Philadelphia, PA: Elsevier; 2021:chap 90. | ||
| ||
Review Date: 10/1/2024 Reviewed By: Kelly L. Stratton, MD, FACS, Associate Professor, Department of Urology, University of Oklahoma Health Sciences Center, Oklahoma City, OK. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. View References The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. No warranty of any kind, either expressed or implied, is made as to the accuracy, reliability, timeliness, or correctness of any translations made by a third-party service of the information provided herein into any other language. © 1997- A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited. | ||


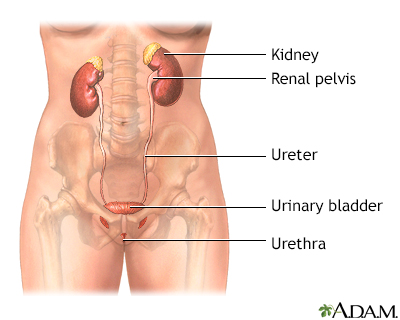 Female urinary tra...
Female urinary tra... Male urinary tract
Male urinary tract
