Subdural hematoma
Definition
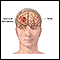
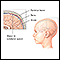
A subdural hematoma is a collection of blood between the covering of the brain (dura) and the surface of the brain.
Alternative Names
Subdural hemorrhage; Traumatic brain injury - subdural hematoma; TBI - subdural hematoma; Head injury - subdural hematoma
Causes
A subdural hematoma is most often the result of a severe head injury. This type of subdural hematoma is among the deadliest of all head injuries. The bleeding fills the brain area very rapidly, compressing brain tissue. This often results in brain injury and may lead to death.
With any subdural hematoma, tiny veins between the surface of the brain and its outer covering (the dura) stretch and tear, allowing blood to collect. In older adults, the veins are often already stretched because of brain shrinkage (atrophy) and are more easily injured.
A chronic subdural hematoma is more often seen in older adults. This type of subdural hematoma may be due to blood that persists after an acute injury or the result of slowly leaking blood. These can occur after a minor head injury and may go unnoticed for many days.
Some subdural hematomas occur without cause (spontaneously).
The following increase the risk for a subdural hematoma:
- Medicines that thin the blood (such as warfarin or aspirin)
- Long-term alcohol use
- Medical conditions that make your blood clot poorly
- Repeated head injury, such as from falls
- Very young or very old age
In infants and young children, a subdural hematoma may occur after child abuse and are commonly seen in a condition called shaken baby syndrome.
Symptoms
Depending on the size of the hematoma and where it presses on the brain, any of the following symptoms may occur:
- Drowsiness, confusion, or coma
- Decreased memory
- Problem speaking or swallowing
- Problems with balance or walking
- Headache
- Seizures or loss of consciousness
- Nausea and vomiting
- Weakness or numbness of arms, legs, face
- Vision problems
- Behavioral changes or psychosis
In infants, symptoms may include:
- Bulging fontanelles (the soft spots of the baby's skull)
- Separated sutures (the areas where growing skull bones join)
- Feeding problems
- Seizures
- High-pitched cry, irritability
- Increased head size (circumference)
- Increased sleepiness or lethargy
- Persistent vomiting
Exams and Tests
Get medical help right away after a head injury. Do not delay. Older adults should receive medical care if they show signs of memory problems or mental decline, even if they don't seem to have an injury.
Your health care provider will ask about your medical history. Your physical exam will include a careful check of your brain and nervous system for problems with:
- Balance
- Coordination
- Mental functions
- Sensation
- Strength
- Walking
If there is any suspicion of a hematoma, an imaging test, such as a CT or MRI scan, will be done.
Treatment
A subdural hematoma is an emergency condition.
Emergency surgery may be needed to reduce pressure within the brain. This may involve drilling a small hole in the skull to drain any blood and relieve pressure on the brain. Large hematomas or solid blood clots may need to be removed through a procedure called a craniotomy, which creates a larger opening in the skull.
Medicines that may be used depend on the type of subdural hematoma, how severe the symptoms are, and how much brain damage has occurred. Medicines may include:
- Diuretics (often given intravenously) and corticosteroids to reduce swelling
- Anti-seizure medicines to control or prevent seizures
Outlook (Prognosis)
The outlook depends on the type and location of head injury, the size of the blood collection, and how soon treatment is started.
Acute subdural hematomas have high rates of death and brain injury. Chronic subdural hematomas have better outcomes in most cases. Symptoms often go away after the blood collection is drained. Physical therapy is sometimes needed to help the person get back to their usual level of functioning.
Seizures often occur at the time the hematoma forms, or up to months or years after treatment. But medicines can help control the seizures.
Possible Complications
Complications that may result include:
- Brain herniation (pressure on the brain severe enough to cause coma and death)
- Persistent symptoms such as memory loss, dizziness, headache, anxiety, and difficulty concentrating
- Seizures
- Short-term or permanent weakness, numbness, difficulty speaking
When to Contact a Medical Professional
A subdural hematoma is a medical emergency. Call 911 or the local emergency number, or go to an emergency room after a head injury. Do not delay.
Spinal injuries often occur with head injuries, so try to keep the person's neck still if you must move them before help arrives.
Prevention
Always use safety equipment at work and play to reduce your risk for a head injury. For example, use hard hats, bicycle or motorcycle helmets, and seat belts. Older individuals should be particularly careful to avoid falls.
References
Kolias AG, Taisic T, Chari A, Hutchinson PJ, Santarius T. Medical and surgical management of chronic subdural hematomas. In: Winn HR, ed. Youmans and Winn Neurological Surgery. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 47.
Papa L, Goldberg SA. Head trauma. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 33.
Stippler M, Mahavadi A. Craniocerebral trauma. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 62.
|
Review Date:
6/13/2024 Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. |