Pregnancy SmartSiteTM
Pregnancy - gestational diabetes; Prenatal care - gestational diabetes DescriptionGestational diabetes is diabetes, defined by high blood sugar (glucose), that starts during pregnancy. If you've been diagnosed with gestational diabetes, learn how to manage your blood sugar so that you and your baby stay healthy. What is Gestational Diabetes?Insulin is a hormone produced in an organ called the pancreas. The pancreas is below and behind the stomach. Insulin is needed to move blood sugar into the body's cells. Inside the cells, glucose is used for energy. Some of it may be stored for later use. Pregnancy hormones can block insulin from doing its job. When this happens, the glucose level may increase in a pregnant woman's blood. In people with gestational diabetes:
How is It Managed?Becoming pregnant when you are at your ideal body weight can help lower your chance of getting gestational diabetes. If you are overweight, try to lose weight before pregnancy. If you do develop gestational diabetes:
What are the Risks of Gestational Diabetes?Women who follow their treatment plan and keep their blood sugar normal or close to normal during their pregnancy should have a good outcome. Blood sugar that is too high raises the risks for:
Checking Your Blood SugarYou can see how well you are doing by testing your blood sugar level at home. Your provider may ask you to check your blood sugar several times each day. The most common way to check is by pricking your finger and drawing a drop of blood. Then, you place the blood drop in a monitor (testing machine) that measures your blood glucose. If the result is too high or too low, you will need to closely monitor your blood sugar level. Your providers will follow your blood sugar level with you. Make sure you know what your blood sugar level should be. Managing your blood sugar can seem like a lot of work. But many women are motivated by their desire to make sure both they and their baby have the best possible outcome. Visits and Tests for You and Your BabyYour provider will closely check both you and your baby throughout your pregnancy. This will include:
If you need insulin or oral medicine to control your blood sugar, you may need to have labor induced 1 or 2 weeks before your due date. After Your DeliveryHigh blood sugar levels often go back to normal after delivery. Still, many women with gestational diabetes develop diabetes within 5 to 10 years after giving birth. The risk is greater in obese women. Women with gestational diabetes should be watched closely after giving birth. They should also continue to get checked at future clinic appointments for signs of diabetes that is persisting. Talk to your provider about measures you can take to reduce your chance of developing diabetes. When to Call the DoctorContact your provider for the following diabetes-related problems:
It's normal to feel stressed or down about being pregnant and having diabetes. But, if these emotions are overwhelming you, call your provider. Your health care team is there to help you. ReferencesACOG Practice Bulletin No. 190: Gestational diabetes mellitus. Obstet Gynecol. 2018;131(2):e49-e64. PMID: 29370047 pubmed.ncbi.nlm.nih.gov/29370047/. American Diabetes Association Professional Practice Committee. 15. Management of diabetes in pregnancy: standards of care in diabetes-2025. Diabetes Care. 2025;48(Supplement_1):S306-S320. PMID: 39651985 pubmed.ncbi.nlm.nih.gov/39651985/. Bodnar LM, Himes KP. Maternal nutrition. In: Lockwood CJ, Copel JA, Dugoff L, et al, eds. Creasy and Resnik's Maternal-Fetal Medicine: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2023:chap 12. Venkatesh KK, Powe CE, Durnwald C, Landon MB. Diabetes mellitus complicating pregnancy. In: Landon MB, Galan HL, Jauniaux ERM, et al, eds. Gabbe's Obstetrics: Normal and Problem Pregnancies. 9th ed. Philadelphia, PA: Elsevier; 2025:chap 45. | ||
| ||
Review Date: 5/22/2025 Reviewed By: LaQuita Martinez, MD, Department of Obstetrics and Gynecology, Emory Johns Creek Hospital, Alpharetta, GA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. View References The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. No warranty of any kind, either expressed or implied, is made as to the accuracy, reliability, timeliness, or correctness of any translations made by a third-party service of the information provided herein into any other language. © 1997- A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited. | ||


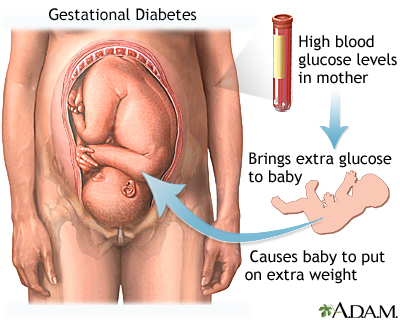 Gestational Diabet...
Gestational Diabet...
