Pregnancy SmartSiteTM
Inflammatory bowel disease - ulcerative colitis; IBD - ulcerative colitis; Colitis; Proctitis; Ulcerative proctitis DefinitionUlcerative colitis is a condition in which the lining of the large intestine (colon) and rectum become inflamed. It is a form of inflammatory bowel disease (IBD). Crohn disease is another form of IBD. CausesThe cause of ulcerative colitis is unknown. People with this condition have problems with their immune system. However, it is not clear if immune problems cause this illness. Stress and certain foods can trigger symptoms, but they do not cause ulcerative colitis. Ulcerative colitis may affect any age group. The peaks in the age of onset occur at ages 15 to 30 and then again at ages 50 to 70. The disease begins in the rectal area. It may stay in the rectum or spread to higher areas of the large intestine. However, the disease does not skip areas. It may involve the entire large intestine over time. Risk factors include a family history of ulcerative colitis or other autoimmune diseases, or Jewish ancestry. SymptomsThe symptoms can be more or less severe. They may start slowly or suddenly. Half of people only have mild symptoms. Others have more severe attacks that occur more often. Many factors can lead to attacks. Symptoms may include:
Children's growth may slow. Other symptoms that may occur with ulcerative colitis include the following:
Exams and TestsColonoscopy with biopsy is most often used to diagnose ulcerative colitis. Colonoscopy is also used to screen people with ulcerative colitis for colon cancer. Other tests that may be done to help diagnose this condition include:
Sometimes, tests of the small intestine are needed to differentiate between ulcerative colitis and Crohn disease, including:
TreatmentThe goals of treatment are to:
During a severe episode, you may need to be treated in the hospital. Your health care provider may prescribe corticosteroids. You may be given nutrients through a vein (IV line). DIET AND NUTRITION Certain types of foods may worsen diarrhea and gas symptoms. This problem may be more severe during times of active disease. Diet suggestions include:
STRESS You may feel worried, embarrassed, or even sad or depressed about having a bowel accident. Other stressful events in your life, such as moving, or losing a job or a loved one can cause worsening of digestive problems. Ask your provider for tips about how to manage your stress. MEDICINES You can take medicine to treat very bad diarrhea. Loperamide (Imodium) can be bought without a prescription. Always talk to your provider before using these drugs. Medicines that may be used to decrease the number of attacks include:
SURGERY Surgery to remove the colon will cure ulcerative colitis and removes the threat of colon cancer. You may need surgery if you have:
Most of the time, the entire colon, including the rectum, is removed. After surgery, you may have:
Support GroupsSocial support can often help with the stress of dealing with illness, and support group members may also have useful tips for finding the best treatment and coping with the condition. More information and support for people with Crohn disease and ulcerative colitis and their families can be found at: www.crohnscolitisfoundation.org Outlook (Prognosis)Symptoms are mild in about one half of people with ulcerative colitis. More severe symptoms are less likely to respond well to medicines. Cure is only possible through complete removal of the large intestine. The risk for colon cancer increases in each decade after ulcerative colitis is diagnosed. Possible ComplicationsYou have a higher risk for small bowel and colon cancer if you have ulcerative colitis. Your provider will recommend a colonoscopy to evaluate for colon cancer at particular intervals. More severe episodes that recur may cause the walls of the intestines to become thickened, leading to:
Problems absorbing nutrients may lead to:
Less common problems that may occur include:
When to Contact a Medical ProfessionalContact your provider if:
PreventionThere is no known prevention for this condition. ReferencesAnanthakrishnan AN, Reguerio MD. Management of inflammatory bowel diseases. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 116. Cameron J. Large bowel. In: Cameron J, ed. Current Surgical Therapy. 14th ed. Philadelphia, PA: Elsevier; 2023:177-286. Galandiuk S, Netz U, Morpurgo E, Tosato SM, Abu-Freha N, Ellis CT. Colon and rectum. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. St Louis, MO: Elsevier; 2022:chap 52. Kaplan GG, Ng SC. Epidemiology, pathogenesis, and diagnosis of inflammatory bowel diseases. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 115. Lichtenstein GR. Inflammatory bowel disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 127. Rubin DT, Ananthakrishnan AN, Siegel CA, Sauer BG, Long MD. ACG clinical guidelines: ulcerative colitis in adults. Am J Gastroenterol. 2019:114(3):384-413. PMID: 30840605 pubmed.ncbi.nlm.nih.gov/30840605/. | ||
| ||
Review Date: 3/31/2024 Reviewed By: Jenifer K. Lehrer, MD, Department of Gastroenterology, Aria - Jefferson Health Torresdale, Jefferson Digestive Diseases Network, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. View References The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. No warranty of any kind, either expressed or implied, is made as to the accuracy, reliability, timeliness, or correctness of any translations made by a third-party service of the information provided herein into any other language. © 1997- A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited. | ||


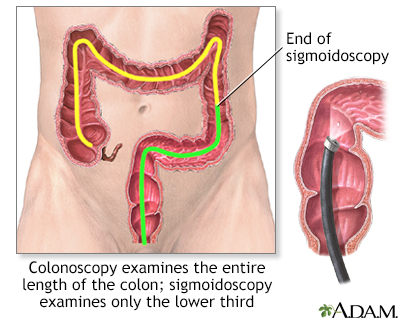 Colonoscopy
Colonoscopy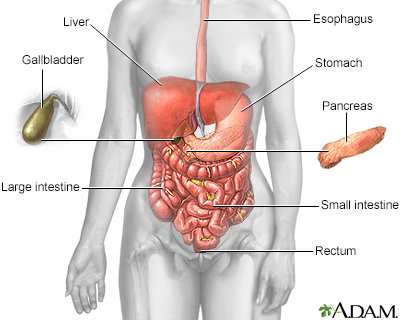 Digestive system
Digestive system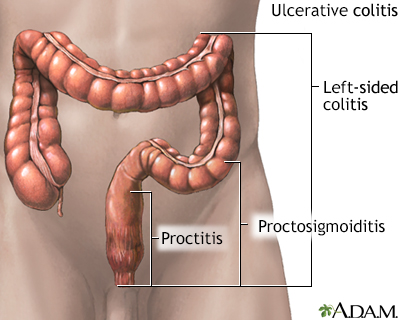 Ulcerative colitis
Ulcerative colitis
