Angiodysplasia of the colon
Definition
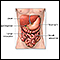
Angiodysplasia of the colon (large intestine) is swollen, fragile blood vessels in the colon. These can result in bleeding and blood loss from the gastrointestinal (GI) tract. Angiodysplasia can also occur in the small intestine with similar causes and symptoms.
Alternative Names
Vascular ectasia of the colon; Colonic arteriovenous malformation; Hemorrhage - angiodysplasia; Bleed - angiodysplasia; Gastrointestinal bleeding - angiodysplasia; G.I. bleed - angiodysplasia; AVM
Causes
Angiodysplasia of the colon is mostly related to the aging and breakdown of the blood vessels. It is more common in older adults. It is almost always seen on the right side of the colon.
Most likely, the problem develops due to normal movement of the colon that causes the blood vessels in the area to enlarge. When this swelling becomes severe, a tiny passageway develops between a small artery and vein. This is called an arteriovenous malformation. Bleeding can occur from this area in the colon wall. Other causes include certain heart and lung conditions.
Rarely, angiodysplasia of the colon is related to other diseases of the blood vessels. One of these is Osler-Weber-Rendu syndrome. The condition is not related to cancer. It is also different from diverticulosis, which is a more common cause of intestinal bleeding in older adults.
Symptoms
The symptoms vary.
Older people may have symptoms such as:
- Weakness
- Fatigue
- Shortness of breath due to anemia
They may not have noticeable bleeding directly from the colon.
Other people may have bouts of mild or severe bleeding in which bright red or black blood comes from the rectum.
There is no pain associated with angiodysplasia.
Exams and Tests
Tests that may be done to diagnose this condition include:
- Angiography 01_003327(only useful if there is active bleeding into the colon).
- CT angiography (CTA). This is a special type of CT scan that shows active bleeding into the intestine.
- Complete blood count (CBC) to check for anemia.
- Colonoscopy.
- Stool test for occult (hidden) blood (a positive test result suggests bleeding from the colon).
Treatment
It is important to find the cause of bleeding in the colon and how fast the blood is being lost. You may need to be admitted to a hospital. Fluids may be given through a vein, and blood products may be required.
Other treatment may be needed once the source of bleeding is found. In most cases, the bleeding stops on its own without treatment.
If treatment is needed, it may involve:
- Angiography to help block the blood vessel that is bleeding or to deliver medicine to help cause the blood vessels to tighten to stop the bleeding.
- Burning (cauterizing) the site of the bleed with heat, argon plasma coagulation, or laser using a colonoscope.
- Medicines: A medicine called octreotide can be injected to help treat the problem.
In some cases, surgery is the only option. You may need the entire right side of the colon (right hemicolectomy) removed if heavy bleeding continues, even after other treatments have been tried. Medicines (thalidomide) may rarely be used to help control the disease in some people.
Outlook (Prognosis)
People who have bleeding related to this condition despite having had colonoscopy, angiography, medicine, or surgery are likely to have more bleeding in the future.
The outlook remains good if the bleeding is controlled.
Possible Complications
Complications may include:
- Anemia
- Death from excessive blood loss
- Side effects from treatment
- Severe loss of blood from the GI tract
When to Contact a Medical Professional
Contact your health care provider if rectal bleeding occurs.
Prevention
There is no known prevention.
References
Kwah J, Brandt LJ. Vascular lesions of the gastrointestinal tract. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology/Diagnosis/Management. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 38.
Ibanez MB, Munoz-Navas M. Occult and unexplained chronic gastrointestinal bleeding. In: Chandrasekhara V, Elmunzer J, Khashab MA, Muthusamy VR, eds. Clinical Gastrointestinal Endoscopy. 3rd ed. Philadelphia, PA: Elsevier; 2019:chap 18.
Reviewed By: Jenifer K. Lehrer, MD, Department of Gastroenterology, Aria - Jefferson Health Torresdale, Jefferson Digestive Diseases Network, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.