Pregnancy SmartSiteTM
Chronic pancreatitis - chronic; Pancreatitis - chronic - discharge; Pancreatic insufficiency - chronic; Acute pancreatitis - chronic DefinitionPancreatitis is swelling of the pancreas. Chronic pancreatitis is present when this problem does not heal or recurs and does not improve, gets worse over time, and leads to permanent damage. CausesThe pancreas is an organ located behind the stomach. It produces chemicals (called enzymes) needed to digest food. It also produces the hormones insulin and glucagon. When scarring of the pancreas occurs, the organ is no longer able to make the right amount of these enzymes. As a result, your body may be unable to digest fat and key elements of food. Damage to the parts of the pancreas that make insulin may lead to diabetes mellitus. The condition is most often caused by alcohol abuse over many years. Repeated episodes of acute pancreatitis can lead to chronic pancreatitis. Genetics may be a factor in some cases. Sometimes, the cause is not known or caused by gall stones. Other conditions that have been linked to chronic pancreatitis:
Chronic pancreatitis is more common in men than in women. This often occurs in people ages 30 to 40. SymptomsSymptoms include:
DIGESTIVE PROBLEMS
Exams and TestsTests to diagnose pancreatitis include:
Tests that may show the cause of pancreatitis include:
Imaging tests that can show swelling, scarring, calcifications or other changes of the pancreas may be seen on:
ERCP is a procedure that looks at your bile and pancreatic ducts. It is done through an endoscope. TreatmentPeople with severe pain or who are losing weight may need to stay in the hospital for:
The right diet is important for people with chronic pancreatitis to keep a healthy weight and get the correct nutrients. A nutritionist can help you create a diet that includes:
The health care provider may prescribe pancreatic enzymes. You must take these medicines with every meal, and even with snacks. The enzymes will help you digest food better, gain weight and reduce diarrhea. Avoiding smoking and drinking alcoholic beverages is very important, even if your pancreatitis is mild. This helps decrease your risk of pancreatitis and pancreatic cancer. Other treatments may involve:
Surgery may be performed if a blockage is found. In severe cases, a part of or the entire pancreas may be removed. Outlook (Prognosis)This is a serious disease that may lead to disability and death. You can reduce the risk by avoiding alcohol. Possible ComplicationsComplications may include:
When to Contact a Medical ProfessionalContact your provider if:
PreventionFinding the cause of acute pancreatitis and treating it quickly may help prevent chronic pancreatitis. Limit the amount of alcohol you drink to reduce your risk of developing this condition. ReferencesForsmark CE. Chronic pancreatitis. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology/Diagnosis/Management. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 59. Forsmark CE. Pancreatitis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 130. Price MD, Walsh CM, Makary MA. Management of chronic pancreatitis. In: Cameron J, ed. Current Surgical Therapy. 14th ed. Philadelphia, PA: Elsevier; 2023:541-545. Van Buren G, Fisher WE. Acute and chronic pancreatitis. In: Kellerman RD, Rakel DP, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2024. Philadelphia, PA: Elsevier; 2024:175-182. | ||
| ||
Review Date: 12/31/2023 Reviewed By: Jenifer K. Lehrer, MD, Department of Gastroenterology, Aria - Jefferson Health Torresdale, Jefferson Digestive Diseases Network, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. View References The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. No warranty of any kind, either expressed or implied, is made as to the accuracy, reliability, timeliness, or correctness of any translations made by a third-party service of the information provided herein into any other language. © 1997- A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited. | ||


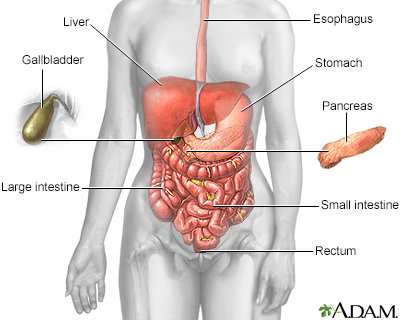 Digestive system
Digestive system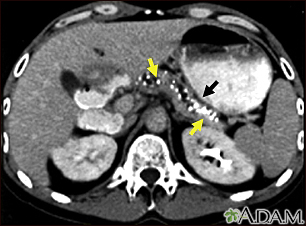 Pancreatitis, chro...
Pancreatitis, chro...
