Pregnancy SmartSiteTM
Bronchial asthma; Wheezing - asthma - adults DefinitionAsthma is a chronic disease that causes the airways of the lungs to swell and become narrow. It leads to breathing difficulty such as wheezing, shortness of breath, chest tightness, and coughing. CausesAsthma is caused by swelling (inflammation) in the airways. An asthma attack occurs when the lining of the air passages has become swollen and the muscles surrounding the airways become tight. This narrowing reduces the amount of air that can pass through the airway. Asthma symptoms can be caused by breathing in substances called allergens or triggers, or by other causes. Common asthma triggers include:
Substances in some workplaces can also trigger asthma symptoms, leading to occupational asthma. The most common triggers are wood dust, grain dust, animal dander, fungi, or chemicals. Many people with asthma have a personal or family history of allergies, such as hay fever (allergic rhinitis) or eczema. Others have no history of allergies. SymptomsAsthma symptoms vary from person to person. For example, you may have symptoms all the time or mostly during physical activity. Most people with asthma have attacks separated by symptom-free periods. Some people have long-term shortness of breath with episodes of increased shortness of breath. Wheezing or a cough may be the main symptom. Asthma attacks can last for minutes to days. An asthma attack may start suddenly or develop slowly over several hours or days. It may become dangerous if airflow is severely blocked. Symptoms of asthma include:
Emergency symptoms that need prompt medical help include:
Exams and TestsYour health care provider will use a stethoscope to listen to your lungs. Wheezing or other asthma-related sounds may be heard. Your provider will take your medical history and ask about your symptoms. Tests that may be ordered include:
TreatmentThe goals of treatment are to:
You and your provider should work as a team to manage your asthma symptoms. Follow your provider's instructions on taking medicines, removing asthma triggers, and tracking symptoms. MEDICINES FOR ASTHMA Your provider may prescribe two kinds of medicines for treating your asthma:
These are also called maintenance or control medicines. They are used to prevent symptoms in people with moderate to severe asthma. You must take these medicines every day for them to work as well as possible. Take them even when you feel OK. Some long-term medicines are breathed in (inhaled), such as steroids and long-acting beta-agonists. Others are taken by mouth (orally). Your provider will prescribe the right medicine for you. These are also called rescue medicines. They are taken:
Tell your provider if you are using quick-relief medicines twice a week or more. If so, your asthma may not be under control. Your provider may change the dose or your daily asthma control medicine to reduce the use of quick-relief medicines. Quick-relief medicines include:
A severe asthma attack requires a visit to your provider. You may also need a hospital stay. There, you will likely be given oxygen, breathing assistance, and medicines given through a vein (IV) or by a nebulizer. ASTHMA CARE AT HOME You can take steps to reduce the chance of asthma attacks:
Asthma action plans are written documents for managing asthma. An asthma action plan should include:
A peak flow meter is a simple device to measure how quickly you can move air out of your lungs.
Outlook (Prognosis)There is no cure for asthma, although symptoms sometimes improve over time, particularly in children. With proper self-care and medical treatment, most people with asthma can lead a normal life. Possible ComplicationsThe complications of asthma can be severe, and may include:
When to Contact a Medical ProfessionalContact your provider for an appointment if asthma symptoms develop. Contact your provider right away if:
Go to the emergency room or call Emergency Medical Services (EMS) right away if these symptoms occur:
PreventionYou can reduce asthma symptoms by avoiding triggers and substances that irritate the airways.
ReferencesBoulet L-P, Godbout K. Diagnosis of asthma in adults. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 51. Cloutier MM, Dixon AE, Krishnan JA, Lemanske RF Jr, Pace W, Schatz M. Managing asthma in adolescents and adults: 2020 asthma guideline update from the National Asthma Education and Prevention Program. JAMA. 2020;324(22):2301-2317. PMID: 33270095 pubmed.ncbi.nlm.nih.gov/33270095/. Drazen JM, Bel EH. Asthma. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 75. Liu AH, Bacharier LB, Fitzpatrick AM, Sicherer SH. Childhood asthma. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 185. Vohra TT, Nowak RM. Asthma. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 59. | ||
| ||
Review Date: 1/1/2025 Reviewed By: Frank D. Brodkey, MD, FCCM, Associate Professor, Section of Pulmonary and Critical Care Medicine, University of Wisconsin School of Medicine and Public Health, Madison, WI. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. View References The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. No warranty of any kind, either expressed or implied, is made as to the accuracy, reliability, timeliness, or correctness of any translations made by a third-party service of the information provided herein into any other language. © 1997- A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited. | ||


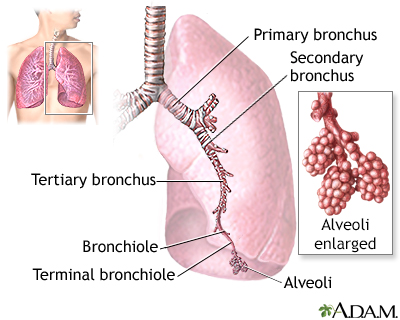 Lungs
Lungs Spirometry
Spirometry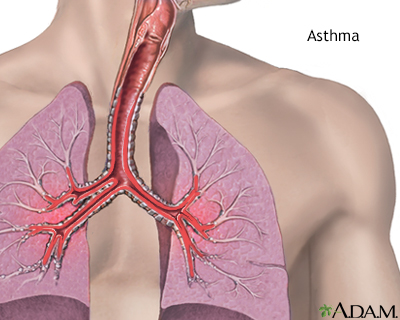 Asthma
Asthma Peak flow meter
Peak flow meter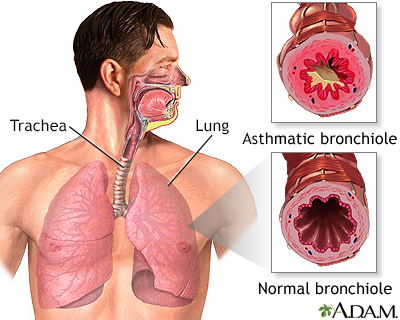 Asthmatic bronchio...
Asthmatic bronchio...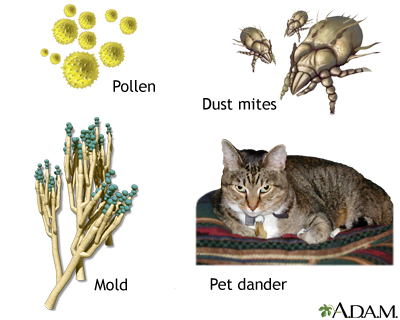 Common asthma trig...
Common asthma trig... Exercise-induced a...
Exercise-induced a...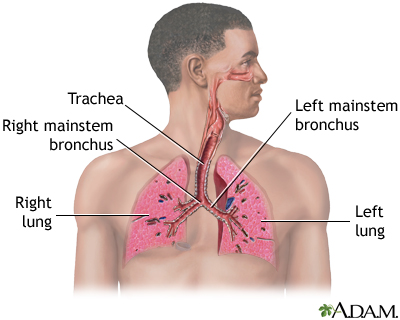 Respiratory system
Respiratory system
